Osteoarthritis (OA) is the most common type of arthritis, especially among older people. OA symptoms vary by the individual. For most people, the disease gets worse over time, particularly if the pain and symptoms aren’t addressed promptly.
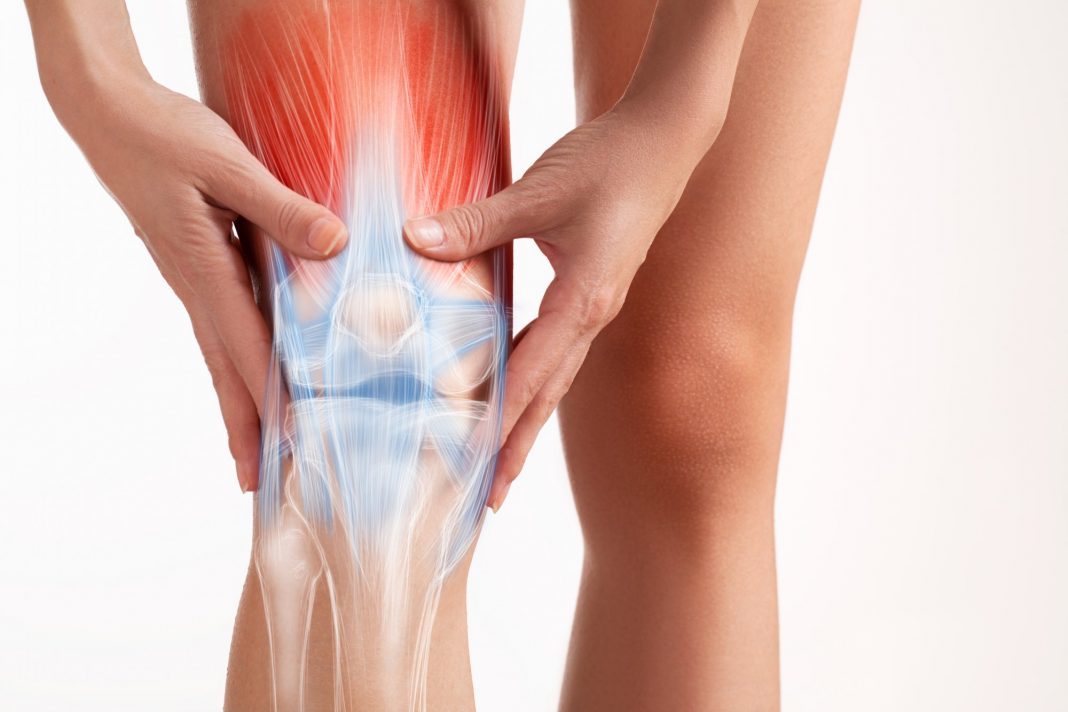
OA mostly affects cartilage, the surface layer of which disintegrates and wears away.
This allows the bones under the cartilage to rub together, causing pain, swelling and progressive loss of motion of the affected joint.
Over time, this deterioration can affect not only the bones but also tendons, ligaments and other aspects of joint health.
The chronic condition affects one in 11 Australians and can cause significant pain, functional impairment and reduced quality of life (QOL).
While there is no cure for OA, the pain and symptoms can be managed through treatment, lifestyle changes and, most importantly, education regarding the identification of the disease and self-care approaches to managing its long-term symptoms.
A lack of knowledge
A recent Australian epidemiological study exploring health literacy in OA has identified gaps in patient understanding of the disease, such as self-care and treatment options. The study also highlights the impact of OA on patients’ QOL and gaps in OA management, including the critical role pharmacists can play in improving a patient’s pain and self-care management.
Head of School and Dean of Pharmacy in the Sydney Pharmacy School at Sydney University, Professor Andrew McLachlan says the global OA burden is rising, with estimates from the Australian Bureau of Statistics showing one in five Australians aged over 45 years will be impacted by the disease.
“Musculoskeletal illness is a significant barrier to quality of life for many people,” he said, adding that this is part of what the study authors are seeking to better understand.
“Osteoarthritis is about stiffness, pain and the discomfort that comes along with pain and inflammation, so the growing burden of disease is really an important prompt for us to figure out what can we do about it and how we, as healthcare professionals, can contribute to ease that burden.
“Among the key findings in our research is the poor health literacy around OA, leading to a lack of awareness … that someone has osteoarthritis. There’s also a lack of understanding regarding the risk factors, such as being overweight.”
If we are to reduce the future burden of OA, there needs to be better awareness of the risk factors and earlier diagnosis and treatment, including self-care.
The Royal Australian College of General Practitioners’ clinical guidelines for the management of knee and hip osteoarthritis encourage patient engagement in self-care.
The guidelines also suggest improved health literacy has the potential to influence the appropriateness of self-management strategies.
They note that patients’ limited engagement with health services and limited ability to understand and interpret OA information affect their decision-making and therefore the appropriateness of the self-care choices they make.
“When considering health literacy, we need to understand it’s more than just knowledge,” Professor McLachlan said.
“It’s actually about patients having access to the information they need, with the information presented in a way they can understand.
“When information is understood, it allows people to appraise it effectively and make a decision about the information’s suitability for them, so it guides what they’re doing when and if they apply it to their own health.
“Early diagnosis and optimal management, including self-care, are critical to addressing the issue of OA, including tailored programs for individuals.”
How can the pharmacist help?
Professor McLachlan says the study pointed out some interesting themes, including that less than four per cent of patients who self-diagnose OA seek advice on pain management from a pharmacist.
“The study revealed that around three in five patients with diagnosable OA may not be actively seeking any medical care and that there’s a low level of involvement of pharmacists in joint pain management.
“Among the study participants, there was also limited self-recognition of osteoarthritis, while knowledge about some of the suitable choices is sub-optimal, which presents an opportunity.
“Pharmacists are best placed to start to have this conversation with people, particularly talking to customers who are self-selecting pain medications, including how to use them safely and appropriately.
“Pharmacists can also help customers identify osteoarthritis pain using a set of five screening questions we’ve developed,” he said.
Screening questions for OA
- How old are you? (Over 45 years indicates the typical onset of OA risk.)
- Do you have painful joints, and do they get worse with activity?
- How do you feel when you wake in the morning? (If people have morning stiffness or longer duration morning stiffness, this will be a cause for referral for other types of musculoskeletal problems.)
- When did the pain first begin? (The answer will indicate whether it’s a chronic issue.)
- What is the level of your pain at its worst, using a one-to-10 scale, and how have you been managing it?
Tips and advice for pharmacy customers
By taking an active role in understanding and treating their conditions, patients will experience less pain and stay more active than those who feel there is nothing they can do.
The Arthritis Australia website highlights the following 10 steps for living well with arthritis:
Take control by knowing your disease. Spend the time to understand what type of arthritis you have and discover the best ways to improve your condition.
Don’t delay, see your doctor. Because arthritis can get worse if left untreated, it’s best to see your doctor as early as possible. Early diagnosis and treatment can limit the effects of arthritis on your life.
Work with your healthcare team and be an important part of it. The best way to live well with arthritis is by working closely with your healthcare team. It may include a variety of healthcare specialists, such as doctors, pharmacists, physiotherapists, occupational therapists and more.
Know about your treatment options. There are many treatments to relieve pain and stiffness and slow the development of arthritis. Work with your healthcare team to find a combination of treatments that best suits your type of arthritis, your symptoms and your lifestyle.
Find new ways to stay active. Regular exercise is one of the most effective treatments for arthritis. It also helps to improve overall health.
Learn techniques to help manage your pain. There are many techniques you can use to cope with pain so that you can go on living your life the way you want to. What works for one person may not work for another, so try different techniques until you find what works best for you.
Acknowledge your feelings and seek support. It’s natural to feel frustrated, angry, scared and even depressed at the prospect of having arthritis. There are many people who can help you deal with the emotional side of arthritis, including family and friends, counsellors or psychologists.
Make food choices that count. There are many myths about food and arthritis. However, no diet has been proven by research to cure arthritis, and there is very little scientific evidence that specific foods have an effect on arthritis.
Balance your life. When you have arthritis, you need to find the right balance between work, activity and rest. Learn how to make the most of your energy and about equipment that can make daily tasks easier.
Call your local state/territory Arthritis Office. Learn about the regular information sessions and arthritis self-management courses run by your local Arthritis Office. These will introduce you to a wide range of skills and small changes you can make that can lessen the impact of arthritis on your life.
To read the full feature as it appears in the October issue of Retail Pharmacy magazine, visit: retailpharmacymagazine.com.au/magazine/retail-pharmacy-october-2021/